One reason for high cholesterol
Apr 08, 2023
In this blog post I will discuss why my cholesterol was 600, and how I lowered it to the low 200s. (No, I did not use statins, as statins do not address the underlying reason WHY cholesterol is high.)
At one point along my health journey, I was told (and convinced) by a carnivore doctor that it was okay to have high cholesterol.
At the time, I was very low carb and frequently fasting. (And very 'stuck' in the dogma that dietary carbohydrates were not needed)
And my total cholesterol was... 600!
I was told that the was okay because I was 'fat adapted' and that I was a 'lean mass hyper responder'.
After discovering and studying the work of Dr. Broda Barnes, Dr. Ray Peat, Dr. Gilbert Ling and others (focused on thyroid and metabolic health), I now realize that my high cholesterol level at that time was just a cry for help from my thyroid.

Now, cholesterol is not BAD.
Cholesterol is vital for the...
- production of hormones
- synthesis of Vitamin D
- production of bile acid
- repair of arterial walls
- protection against inflammation
- and the maintenance of cell structure
And despite messaging from mainstream, lower is *not* better. (ref, ref)
Based on all-cause mortality studies, there is a u-shaped curve when it comes to ideal cholesterol levels. Optimal cholesterol with the lowest all-cause mortality was actually 200-240 mg/dL, which is considered 'borderline high' in mainstream.
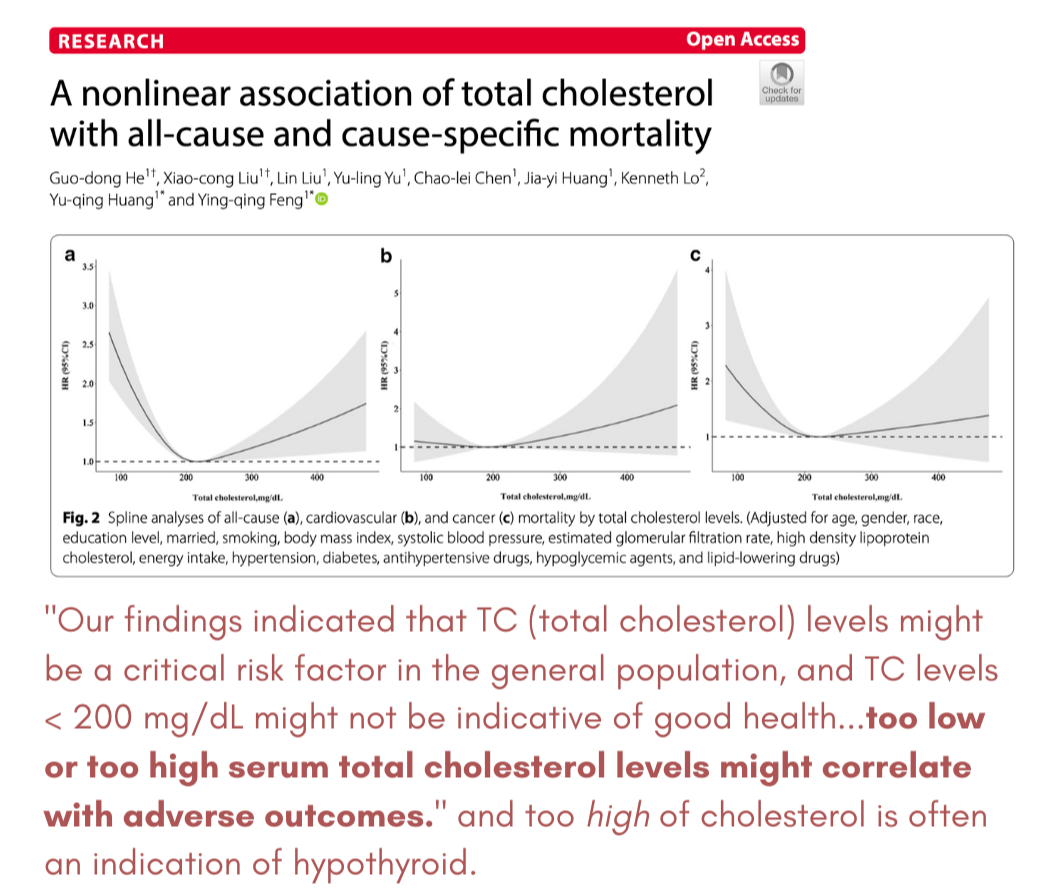
While I do not believe cholesterol should serve as a standalone metric for an overall health assessment, blood cholesterol levels can provide some insight.
While low cholesterol isn't ideal, elevated cholesterol is often a sign of low thyroid function. (ref).
We need active thyroid hormone, T3, and fat soluble vitamins to be able to use cholesterol efficiently, and actually produce the protective steroid hormones. We need T3 to help regulate LDL receptor activity (and thus, play a role in establishing serum cholesterol levels).
Researchers have known this for over 100 years.
The largest population based heart studies showed that cholesterol rises in direct correlation to thyroid function. (ref)
"By 1936, it was clear that hypercholesterolemia in humans and other animals was caused by hypothyroidism, and that hypothyroidism caused many diseased to develop, including cardiovascular disease and cancer." - Dr. Ray Peat
So... how did you lower your cholesterol from 600?
Let's take a look at 3 rounds of bloodwork that measured my total cholesterol level
- August 2019: 600
- June 2020: 262
- March 2022: 210
What changed?
Did I stop eating eggs and red meat?
No.
Repeat after me - eating foods that are high in cholesterol does not raise your cholesterol.
Even the FDA knows this. After fear mongering cholesterol in food, the FDA reversed its stance on dietary cholesterol in 2015, "cholesterol is not a nutrient of concern for overconsumption." (ref)
The current literature does not support the notion that dietary cholesterol increases the risk of heart disease. (ref, ref, ref).
Plus, the work of Dr. Broda Barnes directly connected hypothyroidism with heart disease, and he demonstrated that low cholesterol diets actually made heart disease worse. (ref)
Did I replace my saturated fat consumption with polyunsaturated fatty acids? (PUFAs)
No.
Eating more PUFAs will lower your serum cholesterol, but replacing saturated fats with PUFAs does not reduce CHD events. (ref)
In fact, replacing saturated fat with linoleic acid (an Omega 6 PUFA) was shown to increase the risk of heart attack events (ref). Further, oxidized PUFAs are the bigger concern for increasing risks of adverse coronary events. (ref, ref)
Now you don't need to over consume them, but saturated fats are not the enemy.

Did I take a statin?
No.
Yes, statins lower total cholesterol by blocking its synthesis.
But there are always consequences to isolating certain pathways and symptoms in the body. The body is a system that works together, not a machine with separate parts. When you shut something off, other areas will be impacted.
Consequences of long term statin use include an increased risk of...
- insulin resistance (ref) since statins deplete and interfere with the production of Vitamin K2, which is crucial for proper glucose metabolism (ref)
- diabetes (ref, ref)
- neurological issues (ref, ref)
You can't lower cholesterol synthesis and expect everything else in the body to run smoothly.
Statin use does not address WHY cholesterol is high.
So what changed?
Well, I didn't solely focus on cholesterol. After some lifestyle and dietary changes (and patience), my cholesterol level fell to the 'optimal' range of 200-240. A few other things happened in parallel...
- my T3 (active thyroid hormone) level increased to 4.4
- my body temperature increased from consistently in the 96s
- my TSH lowered to 0.01
In other words, I improved my metabolic and thyroid health. I changed the state of my body. And the lipid levels followed.
Cholesterol should not be used as the stand alone metric for assessing health.
But too high and too low is a sign that something is off.
Work with a doctor to dive a bit deeper - investigate a full thyroid panel, Apo-B levels, LDL particle size, and oxidized LDL levels. What dietary and lifestyle changes can you make to move your health in the right direction?
Artificially lowering your cholesterol and trying to manipulate bloodwork is not the long term answer. Blood lipids are a result of the state your body is in.
We should instead try to improve how the body works as a system, and the improvements in bloodwork will follow.
This is just one of the reasons why we are so adamant on focusing on thyroid and metabolic health. Instead of isolating symptoms and bloodwork into silos, we instead focus on fixing how the body works as a whole system.
And truly one of the simplest (and best) ways to gauge whether you are moving in the right direction at home is to assess body temp and pulse measurements throughout the day. (which is discussed more here).
If you are interested in learning more about improving thyroid and metabolic health, this is what our course, Rooted in Resilience, was designed to do.

